Refractive surgery is a revolutionary approach to correct vision problems and reduce dependency on corrective eyewear. With advancements in medical technology, individuals with refractive errors such as myopia, hyperopia, astigmatism, and presbyopia can benefit from safe and effective surgical procedures. In this comprehensive guide, we will explore the world of refractive surgery, its various techniques, eligibility criteria, potential risks and benefits, post-operative care, and more.
Contents
Introduction to Refractive Surgery

Refractive surgery refers to a collection of surgical procedures aimed at correcting common vision problems such as nearsightedness (myopia), farsightedness (hyperopia), and astigmatism. The primary goal of refractive surgery is to reduce or eliminate the need for glasses or contact lenses, enabling individuals to have clearer vision without visual aids.
There are several types of refractive surgery, each utilizing different techniques to reshape the cornea—the transparent front part of the eye. By altering the cornea’s shape, the surgery modifies how light enters the eye, allowing it to focus correctly on the retina, the light-sensitive layer at the back of the eye.
Types of Refractive Surgery
Here are some common types of refractive surgery:
- LASIK (Laser-Assisted in Situ Keratomileusis): LASIK is the most well-known and frequently performed refractive surgery. During the procedure, a thin flap is created on the cornea using a microkeratome or a femtosecond laser. The surgeon then uses an excimer laser to reshape the underlying corneal tissue. After the reshaping, the flap is repositioned, serving as a natural bandage.
- PRK (Photorefractive Keratectomy): PRK is an older type of refractive surgery that involves removing the thin outer layer of the cornea (epithelium) and using an excimer laser to reshape the underlying corneal tissue. Unlike LASIK, PRK does not involve creating a corneal flap. Instead, the epithelium naturally regenerates over time.
- LASEK (Laser-Assisted Subepithelial Keratectomy): LASEK is similar to PRK, but instead of completely removing the epithelium, it is lifted and preserved as a thin flap. After the corneal reshaping with an excimer laser, the epithelial flap is repositioned.
- SMILE (Small Incision Lenticule Extraction): SMILE is a newer minimally invasive procedure that utilizes femtosecond laser technology. It involves creating a small incision in the cornea and removing a thin, disk-shaped layer of tissue called a lenticule. This reshapes the cornea and corrects the refractive error.
- Implantable Lenses: In some cases, implantable lenses may be used for refractive correction. These include phakic intraocular lenses (IOLs), which are inserted into the eye without removing the natural lens, or clear lens extraction (CLE), where the natural lens is replaced with an artificial intraocular lens.
Eligibility and Post-Operative Assessment

Eligibility for refractive surgery and the pre-operative assessment process are crucial steps to determine if an individual is a suitable candidate for the procedure. Here’s an overview of the eligibility criteria and what to expect during the pre-operative assessment:
Eligibility Criteria
Some eligibility criteria for this surgery are:
- Stable Refractive Error: The individual’s prescription should have remained relatively stable for at least one year. Significant changes in the refractive error can affect the long-term effectiveness of the surgery.
- Age: The minimum age for refractive surgery is typically 18 years old, as the eyes continue to develop until this age. However, some procedures, such as LASIK, may have a minimum age requirement of 21 to ensure stability.
- General Eye Health: The individual should have healthy eyes without any conditions or diseases that could interfere with the surgery or healing process. Conditions like keratoconus, severe dry eye, glaucoma, cataracts, or retinal diseases may disqualify a person from undergoing refractive surgery.
- Corneal Thickness: The cornea needs to have sufficient thickness to allow for the safe removal of tissue during the surgery. Thin corneas may limit the suitability for certain procedures.
- Pregnancy and Nursing: Women who are pregnant or breastfeeding are generally advised to postpone refractive surgery, as hormonal changes during these periods can affect vision stability.
Pre-operative Assessment
The pre-operative assessment is a comprehensive evaluation performed by an ophthalmologist or refractive surgeon to determine the individual’s eligibility and personalize the treatment plan. It typically involves the following:
- Detailed Eye Examination: This includes a thorough assessment of the eye’s health, visual acuity, refractive error measurement, evaluation of corneal curvature, and pupil size.
- Corneal Topography: This test maps the surface curvature of the cornea, helping to detect irregularities, astigmatism, or conditions like keratoconus.
- Pachymetry: This test measures the thickness of the cornea to ensure it is suitable for the chosen procedure.
- Dilated Fundus Examination: The doctor examines the retina and optic nerve to assess the overall health of the back of the eye.
- Tear Film Evaluation: The quantity and quality of tears are assessed to determine if dry eye treatment or management is necessary before surgery.
- Discussion of Expectations and Risks: The surgeon will discuss the individual’s visual goals, potential outcomes, risks, and complications associated with the specific procedure. Realistic expectations are crucial for a satisfactory outcome.
Following the pre-operative assessment, the surgeon will determine if the individual is a suitable candidate for refractive surgery and recommend the most appropriate procedure based on their specific needs and eye characteristics.
Benefits and Risks of Refractive Surgery

Let’s explore the benefits and risks of refractive surgery:
Benefits of Refractive Surgery
- Reduced Dependence on Glasses or Contact Lenses: Refractive surgery aims to correct common vision problems, allowing individuals to have clearer vision without the need for visual aids. Many people experience a significant reduction in their dependence on glasses or contact lenses after successful refractive surgery.
- Convenience and Freedom: Being less reliant on glasses or contact lenses provides convenience and freedom in daily activities, sports, and hobbies. Activities such as swimming, jogging, or playing sports can be enjoyed without worrying about glasses or lenses.
- Improved Quality of Vision: Refractive surgery can often provide improved visual acuity and clarity, enhancing the overall quality of vision. Many individuals report sharper and more vibrant vision after the procedure.
- Quick Recovery: With certain refractive procedures like LASIK or SMILE, the recovery time is relatively quick. Most individuals experience improved vision within a few days or weeks, depending on the procedure.
- Long-Term Results: Refractive surgery typically provides long-lasting results. Once the cornea is reshaped, the effects are permanent, although age-related vision changes may still occur.
Risks and Complications of Refractive Surgery
- Dry Eyes: One of the most common side effects of refractive surgery is dry eyes, which can cause discomfort, irritation, and blurred vision. Dry eye symptoms are usually temporary but can persist in some cases.
- Undercorrection or Overcorrection: While refractive surgery aims to correct the vision to the desired level, there is a possibility of undercorrection (insufficient correction) or overcorrection (overcorrection of the refractive error), leading to residual refractive errors. Enhancements or additional procedures may be required to fine-tune the results.
- Visual Disturbances: Some individuals may experience visual disturbances such as glare, halos, starbursts, or double vision, especially at night or in low-light conditions. These symptoms are usually temporary but may persist in some cases.
- Regression: In certain cases, the cornea may gradually regress toward its original shape, causing a partial loss of the initial correction. This may necessitate further treatment or the use of glasses or contact lenses again.
- Infection and Other Complications: Although rare, there is a small risk of infection, corneal scarring, corneal irregularities, or other complications associated with refractive surgery. Choosing an experienced surgeon and adhering to proper post-operative care can help minimize these risks.
- Unsatisfactory Results: While refractive surgery has a high success rate, some individuals may not achieve their desired level of vision correction. It’s important to have realistic expectations and discuss potential outcomes with the surgeon beforehand.
Post-Operative Care and Follow-up
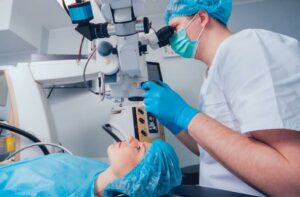
Post-operative care and follow-up appointments are crucial aspects of the refractive surgery process to ensure proper healing, monitor progress, and address any concerns or complications that may arise. Here’s an overview of what to expect in terms of post-operative care and follow-up after refractive surgery:
- Medication and Eye Drops: The surgeon will prescribe antibiotics and anti-inflammatory eye drops to prevent infection and control inflammation during the initial healing period. It’s important to follow the prescribed dosage and frequency as instructed.
- Rest and Recovery: After the surgery, it’s essential to rest your eyes and avoid straining them. Follow the surgeon’s instructions regarding activities to avoid, such as vigorous exercise, swimming, or rubbing your eyes.
- Follow-up Appointments: The surgeon will schedule a series of follow-up appointments to monitor your progress and ensure proper healing. These appointments are typically scheduled within the first few days, weeks, and months following the surgery.
- Vision Check and Adjustment: During the follow-up visits, your visual acuity and overall vision will be assessed to determine the success of the procedure. The surgeon will also check for any residual refractive error and may make adjustments or enhancements if needed.
- Monitoring of the Healing Process: The healing process is unique to each individual. The surgeon will evaluate the corneal healing, and the stability of the correction, and assess any potential complications such as dry eyes, inflammation, or infection.
Conclusion
Refractive surgery offers a transformative solution for individuals with refractive errors, providing improved vision quality and reduced dependency on corrective eyewear. With various surgical techniques available and a high success rate, many people can benefit from this life-changing procedure. However, it is crucial to undergo a thorough pre-operative assessment, choose a reputable surgeon, and follow proper post-operative care to achieve the best possible results.
LASIK eye surgery is a safe 10-minute procedure to help you get rid of glasses. EyeMantra offers the most advanced LASIK options including PRK, Femto Lasik, SMILE surgery, Standard LASIK, ICL, and Contoura vision. If you have any questions on Lasik surgery in Delhi, Lasik surgery cost, and Lasik procedure, call us at 9711116605 or email at [email protected].



п»їbest mexican online pharmacies: cmqpharma.com – п»їbest mexican online pharmacies
mexico drug stores pharmacies
http://cmqpharma.com/# mexican rx online
purple pharmacy mexico price list
online pharmacy india: indian pharmacy online – best india pharmacy
https://canadapharmast.online/# my canadian pharmacy review
Online medicine home delivery [url=https://indiapharmast.com/#]top online pharmacy india[/url] cheapest online pharmacy india
canadian drugs: pharmacy com canada – best canadian online pharmacy
canadian pharmacy cheap: best canadian pharmacy to buy from – pet meds without vet prescription canada
canadian medications: canadapharmacyonline com – reliable canadian pharmacy
http://indiapharmast.com/# indian pharmacy online
pharmacy website india [url=https://indiapharmast.com/#]top online pharmacy india[/url] top online pharmacy india
online shopping pharmacy india: reputable indian pharmacies – indianpharmacy com
best online pharmacy india: buy medicines online in india – world pharmacy india
https://indiapharmast.com/# п»їlegitimate online pharmacies india
mexico drug stores pharmacies: mexican pharmaceuticals online – mexico drug stores pharmacies
cheap canadian pharmacy online: legitimate canadian pharmacies – canadian pharmacy drugs online
indian pharmacy online: buy prescription drugs from india – reputable indian pharmacies
http://ciprodelivery.pro/# ciprofloxacin over the counter
buy amoxicillin: generic amoxicillin cost – buy amoxicillin 500mg usa
http://paxloviddelivery.pro/# buy paxlovid online
ciprofloxacin over the counter [url=http://ciprodelivery.pro/#]buy generic ciprofloxacin[/url] cipro 500mg best prices
http://paxloviddelivery.pro/# paxlovid generic
buy cipro online without prescription: ciprofloxacin 500 mg tablet price – ciprofloxacin generic price
http://clomiddelivery.pro/# can i get cheap clomid prices
paxlovid pharmacy [url=https://paxloviddelivery.pro/#]paxlovid buy[/url] buy paxlovid online
https://clomiddelivery.pro/# where can i buy clomid without insurance
http://paxloviddelivery.pro/# paxlovid for sale
http://ciprodelivery.pro/# cipro 500mg best prices
buy cipro online without prescription [url=https://ciprodelivery.pro/#]ciprofloxacin 500mg buy online[/url] ciprofloxacin generic
ciprofloxacin generic price: buy cipro online canada – buy cipro without rx
http://doxycyclinedelivery.pro/# doxycycline 100 mg price uk
http://amoxildelivery.pro/# amoxicillin over counter
Paxlovid over the counter [url=http://paxloviddelivery.pro/#]Paxlovid buy online[/url] paxlovid pharmacy
https://clomiddelivery.pro/# can you get clomid price
amoxicillin 500 capsule: amoxicillin 500 – amoxicillin 500 mg for sale
https://amoxildelivery.pro/# amoxicillin generic
cost of doxycycline in canada [url=https://doxycyclinedelivery.pro/#]doxycycline 100mg without prescription[/url] doxycycline no script
https://amoxildelivery.pro/# buy amoxicillin 500mg usa
paxlovid cost without insurance: paxlovid india – paxlovid for sale
https://doxycyclinedelivery.pro/# doxycycline buy canada
doxycycline hyclate 100 mg cap [url=https://doxycyclinedelivery.pro/#]doxycycline capsules[/url] doxycycline cost india
http://amoxildelivery.pro/# buy amoxicillin online no prescription
https://amoxildelivery.pro/# amoxicillin over the counter in canada
https://clomiddelivery.pro/# where can i buy generic clomid without insurance
amoxicillin in india [url=https://amoxildelivery.pro/#]amoxicillin 500mg capsules[/url] amoxicillin 500mg capsules
can i order generic clomid online: cost clomid without insurance – buying generic clomid without dr prescription
paxlovid covid: paxlovid for sale – paxlovid price