Vision problems can have a significant impact on a person’s quality of life, making it difficult to perform everyday tasks and limiting their ability to enjoy activities. While glasses and contact lenses can provide temporary solutions, they may not be ideal for everyone. In such cases, surgical procedures like keratectomy may be an option. This blog will provide an overview of keratectomy, its types, the things to consider before and after the procedure, and potential complications, to help readers make an informed decision.
Contents
What Is Keratectomy?
Keratectomy refers to a surgical procedure that involves removing a portion of the cornea, which is the clear outermost layer of the eye. The procedure is typically used to correct refractive errors in vision, such as myopia (nearsightedness) and astigmatism. Keratectomy can be performed using a variety of techniques, including photorefractive keratectomy (PRK), laser-assisted sub-epithelial keratectomy (LASEK), and laser in situ keratomileusis (LASIK).
Types Of Keratectomy Procedures
Several types of keratectomy procedures are commonly used to treat various vision problems. Here are some of the most common types:
Photorefractive keratectomy (PRK)
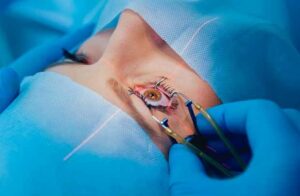 PRK is a type of laser eye surgery that involves removing the surface layer of the cornea (epithelium) and using a laser to reshape the underlying corneal tissue. The laser is used to remove a precise amount of tissue from the cornea, changing its shape and correcting the refractive error that causes vision problems such as myopia, hyperopia, and astigmatism. The epithelium naturally grows back over a few days to a week.
PRK is a type of laser eye surgery that involves removing the surface layer of the cornea (epithelium) and using a laser to reshape the underlying corneal tissue. The laser is used to remove a precise amount of tissue from the cornea, changing its shape and correcting the refractive error that causes vision problems such as myopia, hyperopia, and astigmatism. The epithelium naturally grows back over a few days to a week.
PRK is typically recommended for patients with thinner corneas or who are not good candidates for LASIK, and it can be an effective option for treating low to moderate levels of nearsightedness, farsightedness, and astigmatism. However, the recovery time can be longer than with other procedures, and some patients may experience discomfort or blurry vision during the initial healing period.
Laser-assisted subepithelial keratectomy (LASEK)
LASEK is similar to PRK, but instead of removing the epithelium, the surgeon lifts the thin flap using a special solution. The laser is then used to reshape the cornea, and the flap is replaced and smoothed out. Because the epithelium remains attached, it may take a little longer to heal than with PRK, but there is generally less discomfort and faster visual recovery.
LASEK may be a good option for patients with thinner corneas or who have a higher risk of complications with LASIK, and it can be effective for treating mild to moderate levels of myopia, hyperopia, and astigmatism.
Laser in situ keratomileusis (LASIK)
LASIK is one of the most common types of keratectomy procedures. It involves creating a flap in the cornea using a microkeratome (a small blade) or a femtosecond laser. The flap is then lifted, and a laser is used to reshape the underlying corneal tissue before the flap is replaced and smoothed out.
LASIK is generally a quick and painless procedure that can correct a range of vision problems, including myopia, hyperopia, and astigmatism. The recovery time is typically fast, with most patients experiencing improved vision within a day or two.
Epi-LASIK
Epi-LASIK is similar to LASEK, but a specialized instrument is used to separate the epithelium from the cornea. The epithelium is then lifted, and the laser is used to reshape the underlying corneal tissue. The epithelium is then replaced and smoothed out.
Epi-LASIK may be a good option for patients with thin or irregular corneas, and it can be effective in treating mild to moderate levels of myopia, hyperopia, and astigmatism.
Automated lamellar keratectomy (ALK)
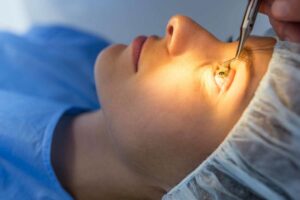 ALK is an older type of keratectomy procedure that involves creating a thin flap of the cornea using a microkeratome. The flap is then lifted, and a laser is used to reshape the underlying corneal tissue before the flap is replaced.
ALK is an older type of keratectomy procedure that involves creating a thin flap of the cornea using a microkeratome. The flap is then lifted, and a laser is used to reshape the underlying corneal tissue before the flap is replaced.
ALK is not as commonly used today, as newer procedures like LASIK and PRK have shown to be more effective and safe in treating vision problems. However, it may still be an option for some patients with thicker corneas and higher levels of nearsightedness.
It’s important to note that while keratectomy procedures can be effective in correcting vision problems, they do carry some risks and potential complications. It’s important to discuss the potential benefits and risks of each procedure. Each of these procedures has its advantages and disadvantages, and the best option for a particular patient depends on their individual needs and circumstances.
Is Keratectomy A Painful Procedure?
Keratectomy procedures typically involve local anesthesia. This means that the eye gets numb before the procedure begins. This helps to prevent pain or discomfort during the surgery itself. Patients may experience some mild discomfort or pressure during the procedure. But this is usually manageable with medication.
After the procedure, it’s normal to experience some discomfort or irritation in the treated eye, including dryness, redness, and sensitivity to light. The level of discomfort can vary depending on the type of keratectomy procedure performed and the individual patient’s pain tolerance.
Pain medication and eye drops help the patients manage any discomfort after the procedure. It’s important to follow the post-operative instructions provided by the surgeon carefully, including using eye drops as directed and avoiding activities like swimming and strenuous exercise until the eye has fully healed.
Overall, while keratectomy procedures may cause some mild discomfort or irritation, the use of local anesthesia and post-operative pain management measures can help to minimize any pain or discomfort experienced by patients.
Things To Consider Before Keratectomy Surgery
 Here are some important factors to keep in mind:
Here are some important factors to keep in mind:
- Consultation with an ophthalmologist: The first step in considering a keratectomy surgery is to schedule a consultation with an experienced ophthalmologist. The surgeon will evaluate the patient’s eye health and vision needs to determine if keratectomy is a suitable treatment option.
- Patient’s overall health: Patients should inform their surgeon of any pre-existing medical conditions, allergies, or medications they are currently taking. Certain medical conditions or medications can affect the patient’s eligibility for surgery.
- Realistic expectations: Patients need to have realistic expectations about what keratectomy surgery can achieve. While it can correct many vision problems, it may not provide perfect vision. There is a chance that additional treatment may be required in the future.
- Cost: Keratectomy procedures can be expensive, and insurance may not cover the full cost. Patients should discuss the cost of the procedure with their surgeon and their insurance provider before undergoing surgery.
Complications After Keratectomy
Keratectomy procedures are generally safe, but like any surgical procedure, there are potential risks and complications. Here are some of the possible complications that can occur after keratectomy:
- Infection, such as redness, swelling, and discharge from the eye.
- Vision problems, such as halos, glare, and decreased visual acuity.
- Corneal haze, a cloudy or hazy appearance.
- Dry eyes, discomfort, and irritation.
- Astigmatism
- Corneal thinning in rare cases.
Tips And Precautions After Keratectomy
 After undergoing a keratectomy procedure, there are several tips and precautions that patients should follow to ensure proper healing and minimize the risk of complications. Here are some important things to keep in mind:
After undergoing a keratectomy procedure, there are several tips and precautions that patients should follow to ensure proper healing and minimize the risk of complications. Here are some important things to keep in mind:
- Follow the surgeon’s instructions: Patients should carefully follow the post-operative instructions provided by their surgeon. This may include using prescribed eye drops, avoiding rubbing or touching the eyes, and avoiding activities like swimming and strenuous exercise.
- Rest and avoid strenuous activity: One should rest and avoid any strenuous activity for a few days after the procedure. This can allow the eyes to heal properly.
- Wear protective eyewear: It is important to wear protective eyewear, such as sunglasses or goggles. This is to protect the eyes from bright sunlight, wind, and dust.
- Avoid getting water in the eyes: One should avoid getting water in the eyes for several days after the procedure. This can increase the risk of infection.
- Inform healthcare providers: It is important to inform any other healthcare providers that they have undergone a keratectomy procedure.
- Avoid rubbing or touching the eyes: Patients should avoid rubbing or touching the eyes. This can cause irritation or infection.
By following these tips and precautions, patients can minimize the risk of complications and ensure proper healing after undergoing a keratectomy procedure.
Conclusion
Keratectomy is a surgical procedure that can correct various vision problems. It involves removing a portion of the cornea to reshape it and improve visual acuity. While keratectomy is generally safe, there are potential risks and complications. Hence, the patients should carefully consider the procedure before undergoing it. By following post-operative instructions and attending follow-up appointments, patients can ensure proper healing and minimize the risk of complications. If you are considering keratectomy, consult with an experienced ophthalmologist to determine if it’s the right option for you and seek help for any concerns or questions you may have.
LASIK surgery is a safe 10-minute procedure to help you get rid of glasses. EyeMantra offers the most advanced LASIK options including PRK, Femto Lasik, SMILE surgery, Standard LASIK, ICL, and Contoura vision. If you have any questions on Lasik surgery in Delhi, Lasik surgery cost, and Lasik procedure, call us at 9711116605 or email at [email protected].



Hey there this is somewhat of off topic but I was wanting to know if blogs use WYSIWYG editors or if you have to manually code with HTML. I’m starting a blog soon but have no coding knowledge so I wanted to get advice from someone with experience. Any help would be greatly appreciated!
Awesome blog! Is your theme custom made or did you download it from somewhere? A design like yours with a few simple tweeks would really make my blog shine. Please let me know where you got your theme. Kudos Miss Samsung Fascinate
Hey there just wanted to give you a quick heads up and let you know a few of the pictures aren’t loading correctly. I’m not sure why but I think its a linking issue. I’ve tried it in two different internet browsers and both show the same outcome.
I was looking at some of your blog posts on this website and I believe this web site is real instructive! Keep posting .
Hello gentleman do you’ve got new links ? I enjoy article evolve for my friend ‘ ..
Hello! I simply would want to supply a large thumbs up with the excellent info you’ve here on this post. We are coming back to your blog site for much more soon.